MUTATIONS
and the COVID-19
Novel Coronavirus
September 2020
Mutations in the natural world are normal and most happen without any real consequence. They are random and they are accidents. Unfortunately, the word itself has a bad connotation. The truth is that mutations have always been very important in creating the amazing diversity of the evolution of life.
In essence, we and every other living organism on the planet are mutants! When using the term mutant in reference to COVID-19 (which is also a mutant), it is important to understand how mutations arise and what they really mean in relation to a virus such as the novel coronavirus, in order to assuage our anxiety when we are told the COVID-19 coronavirus is mutating.
MUTATIONS ARE MISTAKES
Mutations are caused by mistakes the polymerase molecule (the enzyme found in every living thing that makes long chains of repeated units) sometimes makes when copying long strings of letters, such as those in our DNA.
Just as a typist relies on spellcheck and the backspace key or a proofreader, most of these mistakes are corrected. But still, some go uncorrected and these mistakes are called mutations.
Mutations can have negative effects or they may have some beneficial effects to the survival of the organism, and some may have no effect at all on the living thing. Of course, mutations can also arise from other sources in our environment such as high-energy light waves (ultraviolet light, X-rays, gamma rays, etc.), many metals, certain chemicals, and certain viruses and bacteria, etc.
MUTATIONS IN DNA
Our DNA (Deoxyribonucleic acid) is a blueprint or recipe of instructions to make proteins. But only small parts of our DNA, called genes, actually code for proteins.
There are also many other regions of our DNA, some of which regulate how many proteins get made and others which have no known function at the moment. Should a mutation arise in one of those unknown regions, nothing (at least as far as we know) happens.
OUR DNA CODE COMES WITH REDUNDANCIES
Our DNA Code has redundancies built into it to keep mistakes (mutations) to a minimum.
The following is a simplified explanation of a DNA code:
Three sequential letters are equivalent to one specific protein building block in the code. For example, GGC tells the cell to reach for a glycine to add to the growing protein chain. But GGA also means glycine. Thus, it is apparent that the third letter is inconsequential because the DNA code has redundancies.
So if the DNA mutates from GGC to GGA, the protein will look the same. But if the mutation turns GGC into ABC, the cell will add a different building block altogether, which may affect how the protein performs.
The above example is of a mutation affecting one letter, but there are all kinds of mutations, like insertions, deletions, and massive changes that can wreak a lot of havoc.
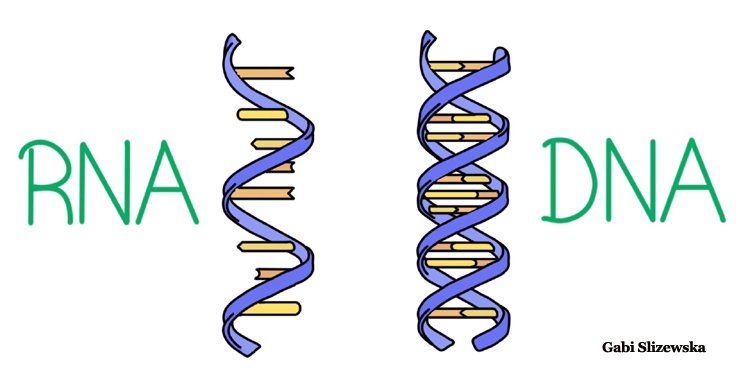
RNA vs DNA
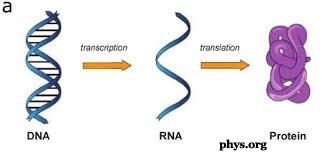
In humans and other mammals, our DNA contains genetic instructions that are copied into our RNA (Ribonucleic acid). The DNA stays in the cell's nucleus and the RNA then carries the copies of genetic information to the rest of the cell through a process that forms the proteins that carry out our bodily functions.
Viruses such as the coronavirus also have a genetic blueprint. But, unlike in humans and other mammals, the genetic material for these coronaviruses is encoded in RNA only.
The coronavirus also has a polymerase to make copies of its RNA so that each new viral particle can carry this blueprint. Unfortunately, this polymerase makes mistakes and mutations arise that are not corrected, just like with the polymerase that codes our DNA.
When the coronavirus RNA gets into our cells, it causes the protein synthesis machinery of our cells to mistake it for the RNA produced by our own DNA.
With most viruses, a sample will show that
the RNA of all the viral particles is slightly different. These are mutations that
are normal. This is because when mutations arise, they may not have any appreciable impact on
the virus. But many diseases can occur when these mutations go awry!
NEW YORK TIMES GRAPHIC
A graphic created by the New York Times illustrates how the coronavirus that causes COVID-19 enters the body and attaches to our cells. Once inside our cells, it releases its RNA. Our hijacked cells serve as virus factories, reading the virus's RNA and making viral proteins to compromise the immune system. The virus then assembles new copies of itself and spreads to more parts of the body and by way of saliva, sweat, and other bodily fluids, to other humans.
Please click here to see the graphic. Below is the content:
The SARS-CoV-2 Coronavirus-(COVID-19)
The virus that causes Covid-19 is currently spreading around the world. At least six other types of coronaviruses are known to infect humans, with some causing the common cold and two causing outbreaks: SARS and MERS.
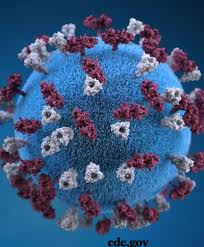
Covered with Spikes
The coronavirus is named after the crownlike spikes that protrude from its surface. The virus is enveloped in a bubble of oily lipid molecules, which falls apart on contact with soap.
Entering a Vulnerable Cell
The virus enters the body through the nose, mouth or eyes, then attaches to cells in the airway that produce a protein called ACE2. The virus is believed to have originated in bats, where it may have attached to a similar protein.
Releasing Viral RNA
The virus infects the cell by fusing its oily membrane with the membrane of the cell. Once inside, the coronavirus releases a snippet of genetic material called RNA.
Hijacking the Cell
The virus’s genome is less than 30,000 genetic “letters” long. (Ours is over 3 billion.) The infected cell reads the RNA and begins making proteins that will keep the immune system at bay and help assemble new copies of the virus.
Making Viral Proteins
As the infection progresses, the machinery of the cell begins to churn out new spikes and other proteins that will form more copies of the coronavirus.
Assembling New Copies
New copies of the virus are assembled and carried to the outer edges of the cell.
Spreading the Infection
Each infected cell can release millions of copies of the virus before the cell finally breaks down and dies.
Immune Response
Most Covid-19 infections cause a fever as the immune system fights to clear the virus. In severe cases, the immune system can overreact and start attacking lung cells. The lungs become obstructed with fluid and dying cells, making it difficult to breathe. A small percentage of infections can lead to acute respiratory distress syndrome, and possibly death.
Leaving the body
Coughing and sneezing
can expel virus-laden droplets onto nearby people and surfaces, where the virus
can remain infectious for several hours to several days. The C.D.C. recommends
that people diagnosed with Covid-19 wear masks to reduce the release of viruses. Health care workers and others who care for
infected people should wear masks, too.
A Possible Vaccine
A future vaccine could help the body produce antibodies that target the SARS-CoV-2 virus and prevent it from infecting human cells. The flu vaccine works in a similar way, but antibodies generated from a flu vaccine do not protect against coronavirus.
How Soap Works
Soap destroys the virus when the water-shunning tails of the soap molecules wedge themselves into the lipid membrane and pry it apart.
The best way to avoid getting infected with the coronavirus is to wash your hands with soap, avoid touching your face, keep your distance from sick people and regularly clean frequently used surfaces.
Please note: This New York Times article was published on March 13, 2020. As we continue to learn about the COVID-19 coronavirus, some of this information may have to, or have been, updated. Regardless, the graphic contains important information about the coronavirus broken down into a simplified visual presentation.
TAKE AWAY...
MUTATIONS ARE ACCIDENTS
It is most important to remember that mutations are just accidents. The accidents can be happy ones and some of these random mutations may end up helping a virus. But a virus does not have a brain, is not clever, and most mutations are neither good nor bad because they do not affect the code or recipe that carries the instructions on how to make a protein.
VIRUS MUTATIONS THAT MAKE A DIFFERENCE
The new coronavirus is an example of some mutations that do make a difference. The new virus needed to mutate in order to become good at infecting humans.
It certainly could be possible that in the future a mutation could arise in a gene that codes for the external part of the coronavirus, the part that gets recognized by our immune system as foreign. It would thus create a new strain of the virus to which we would not yet be immune. This happens a lot with RNA viruses. Luckily, it has not happened yet with the COVID-19 coronavirus and so far it appears to be genetically stable.
WHAT DO MUTATIONS MEAN FOR THE DEVELOPMENT OF AN EFFECTIVE VACCINE?
How viruses mutate will determine whether or not a vaccine can be developed that will be effective. When a virus passes from person to person, it is mutating. That means there are going to be some changes in the virus’s genetic code. But most mutations don’t change how the virus functions.
A virus enters a cell, hijacks the cell’s machinery and uses it to make many copies of itself. During these replications, small errors or mutations can occur. Those mutations accumulate over time as the virus spreads from cell to cell and person to person.
Traditional vaccines work because they use inactivated antigens (virus proteins) to prompt the body to develop antibodies which bind to specific protein spots (antigens)on a virus. The antibodies can then neutralize the virus. If the mutations the virus has gone through do not affect this interaction, the vaccine hopefully won’t need constant updating. But if the virus has mutated in a way that has altered the shape of an antigen, it will be very difficult to develop a long-lasting universal vaccine.
TRADITIONAL VACCINES vs
RNA VACCINES
As noted above, traditional vaccines against viruses inject the body with inactivated virus proteins called antigens. The antigens stimulate the body's immune system to recognize the specific virus and produce antibodies in response, with the hope that these antibodies will fight against future virus infection.
RNA vaccines, on the other hand, do not introduce an antigen, but instead inject a short sequence of the virus's RNA. This messenger RNA provides cells with instructions to produce the virus antigens themselves.
While no RNA vaccines have yet been approved in advanced vaccine trials, these vaccines have an advantage over traditional vaccines in that they would be easier and quicker to produce, and would allow the body to generate a more natural response to a virus.
THE MEASLES VACCINE
The measles vaccine is an example of an effective vaccine. Even though the measles virus mutates as fast as the flu and the COVID-19, the measles vaccine from 1950 is still effective today.
The reason for the continued efficacy of the measles vaccine is because the measles virus uses certain proteins to enter a cell that cannot mutate even slightly without breaking and the measles vaccine targets those parts. The measles vaccine effectively corners and destroys the measles virus.
THE FLU VACCINE &
THE MANY STRAINS OF THE FLU
The way in which the flu virus mutates its antigens allows the virus to evolve into different strains. If a person is infected by Strain A, the immune system is able to recognize that strain but then the virus is able to mutate its antigens in such a way that it can still perform its function but the antibodies against Strain A are no longer able to recognize Strain B. Thus the antibodies produced by the vaccine for one strain can’t bind to the other and the vaccine becomes ineffective.
Each different strain requires a slightly different vaccine. New vaccines are continuously being developed to target the new flu strains. Unfortunately, the flu vaccines only offer partial immunity to the different flu strains that appear each year.
POPULATION OR HERD IMMUNITY & NEW STRAINS OF VIRUSES
Some viruses can respond to the immunity in the population they are trying to infect and if people become immune to the dominant strain (either by fighting off the virus or through vaccination), versions of the virus with mutations that get around the population’s immunity are more likely to spread and then can develop into new strains.
COVID-19 is a brand new virus so there is no widespread immunity to it. There are very few immune hosts who could stop it from spreading and since it doesn’t need to change to survive, any mutations that could modify the shape of its antigens are rare.
At this point in time, even though scientists know of at least 11 mutations which have become fairly common, it appears to be the same virus infecting people worldwide. This means that it may be that only one strain of the virus exists at this time (as of this writing).
The spike protein of the COVID-19 coronavirus is the one which allows the virus to infect cells in the throat and lungs. This protein has changed very little up to this point, making some scientists believe that the virus cannot alter itself much and still remain infectious.
Update: Now we know the COVID-19 coronavirus is indeed capable of producing new strains. As of March of 2021, there are three vaccines available in the US and the race to vaccinate as many people as possible is well on its way. Unfortunately, some of the strains may not be recognized by the available vaccines.
THE RACE TO CONQUER COVID-19 CONTINUES WORLDWIDE
So much more research must be done concerning the coronavirus, how it spreads, if those who have been infected become immune, and if so, how long will that immunity last, etc. In the meantime, we all need to be cautious and keep informed.
Wearing masks in public, keeping social distances of at least 6 feet from others, washing and sanitizing our hands regularly, meeting in very small groups, and isolating if we come in contact with an infected person appear to be the best advice available.
The key to the public health response for the future must be to continue monitoring the variants as they appear and measure their characteristics. Scientists will be able to use this information to develop appropriate methods such as new vaccines that will be effective against the new variants.
Please note: Much scientific information about mutations came from the McGill University Office for Science and Society.
"The Cleanest Clean You've Ever Seen."
by
ABC Oriental Rug & Carpet Cleaning Co.
130 Cecil Malone Drive Ithaca, NY 14850
607-272-1566
Recent COVID-19 Articles:
~~~~~~
~~~~~~
~~~~~~
Soaps, Sanitizers, and Disinfectants
~~~~~~
~~~~~~
~~~~~~
GIVE THE
GIFT OF CLEAN!

Why not think 'outside the box' and give
a Gift Certificate for professional carpet, upholstery, or tile
& grout cleaning from ABC for any special occasion!
Does a special person have a favorite area rug or oriental rug that needs cleaning or repair? Just give us a call. You'll make their day!
Bring in the mats from a car and we'll clean them as well.
Contact
us if you live in the Ithaca, NY or surrounding areas and we will
tailor a special gift certificate just for you for any Special Occasion.
We would love to send our monthly newsletter directly to YOUR INBOX.
Just sign up below...
(Your email is safe with us. Your privacy is our priority.)
Viewing Us on Mobile?
Text to Join Below...


ABC Oriental Rug & Carpet Cleaning Co.
is a FOUNDING MEMBER of the
Association
of Rug Care Specialists.
"To Teach, Cultivate and Advance the Art and Science
of Rug Care"

The Standard of Excellence